Employee Benefits Market Check Survey: What Employers Are Watching in EB
As the employee benefits landscape grows more intricate, employers are under constant pressure to manage rising costs, ensure compliance, and meet the evolving expectations of a diverse workforce. With a seemingly endless array of strategies, technologies, vendors, and plan designs to consider, making the right decisions can feel overwhelming. Amid this complexity, many employers are stepping back to take a more strategic, forward-looking approach.
We conducted a poll on July 21 to capture employer perspectives on the evolving employee benefits space. The results are summarized below.
How do you see your employee benefits strategy evolving over the next 3-5 years?
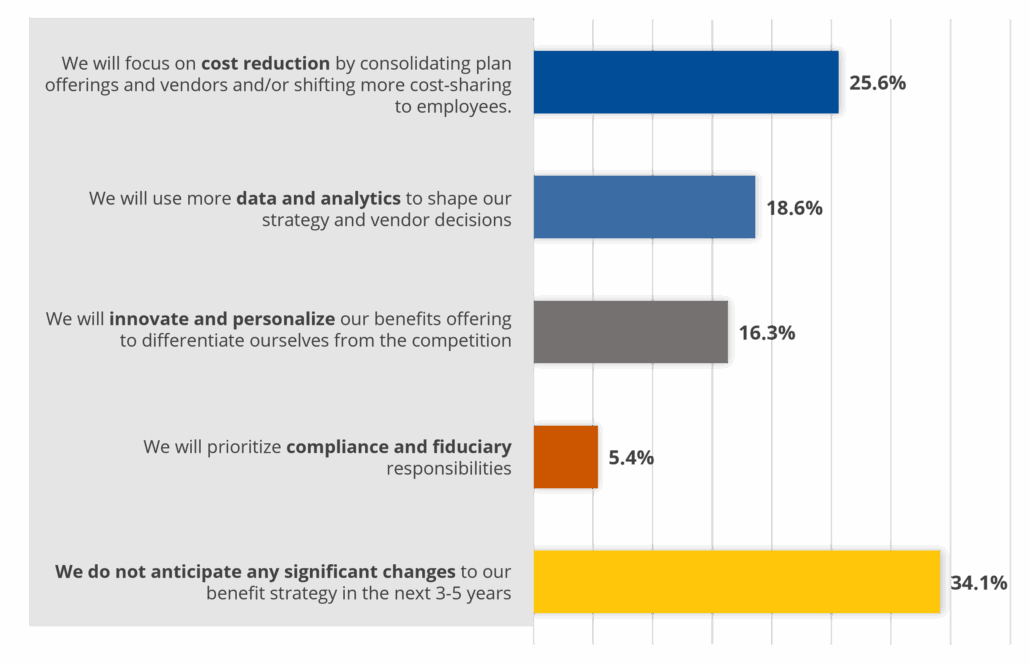
*Results based on 129 employer respondents.
What Trends in Employee Benefits Are You Monitoring Most Closely? (Open-Ended Question)
Responses were normalized and categorized into common themes to identify the most frequently mentioned trends across open-ended employer feedback.
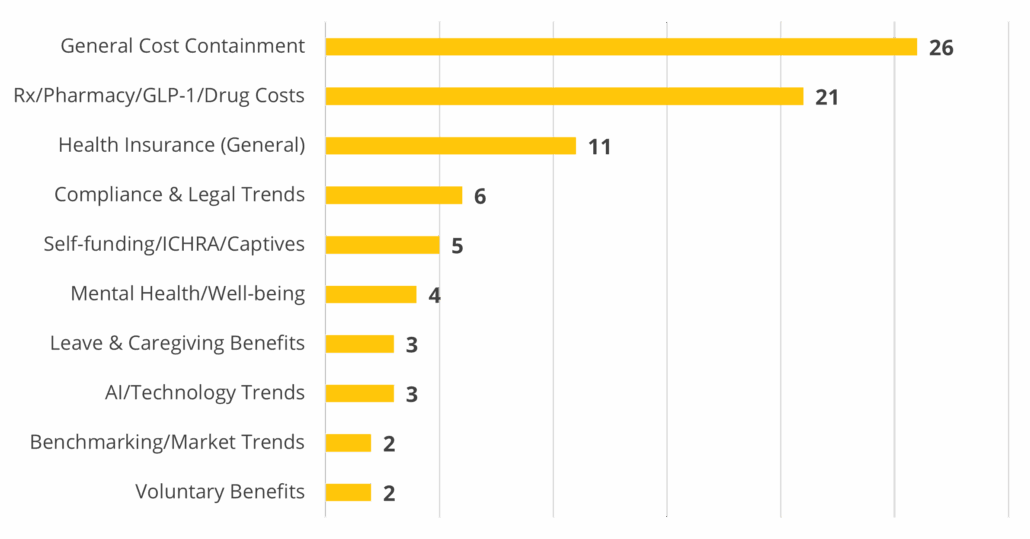
Response Highlights

Key Findings
Employers are facing a benefits landscape marked by increasing complexity, rising costs, and evolving employee expectations. Across both questions — what trends they’re monitoring and how they see their benefits strategy evolving — cost containment emerged as the dominant theme for employers, particularly related to health insurance premiums and pharmacy spend. High-cost therapies such as GLP-1 medications were frequently cited, alongside concerns about out-of-pocket costs, plan design, and stop-loss claims. Some employers are actively exploring strategies such as self-funding, ICHRA models, and reference-based pricing to manage financial risk. Meanwhile, a smaller but notable number are paying close attention to compliance with federal and state regulations, signaling ongoing concern over the administrative and legal complexity of benefits programs.
Beyond cost, several employers are looking ahead and prioritizing more flexible, personalized benefits, a theme reflected in both the open-ended comments and the multiple-choice responses. Mental health, caregiving support, and voluntary benefits were highlighted as areas of growing interest. Others mentioned the potential role of AI and technology in shaping future strategy, especially in relation to plan management, employee experience, and internal consulting capabilities.
Key Takeaways for Employers:
- Prioritize cost transparency and control, especially around Rx spend, high claims, and specialty medications.
- Explore benefit models such as ICHRA, captives, alternative provider networks, and self-funding to increase flexibility and financial sustainability.
- Keep a pulse on employee needs as mental health, financial planning, family support, and ease of access continue to rise in importance.
- Stay ahead of regulatory shifts, particularly in multi-state environments or industries with rapidly changing compliance requirements.
- Use data and analytics not only for cost control but also to support better plan design, additional products, engagement, and outcomes.
Should you have any questions regarding any of this information or want to discuss your employee benefits strategy, please contact your local Assurex Global adviser.
For additional insight into some of the topics covered here, we invite you to visit some of our other Market Check Surveys:



Leave a Reply
Want to join the discussion?Feel free to contribute!